Roseanne Gichuru, DO, MBA
Download: Hysterectomy FAQ_FFHA2020
Hysterectomy – the surgical removal of the uterus—is one of the most common gynecologic surgeries performed today. The procedure is done for many reasons including:
- abnormal uterine bleeding
- fibroids
- endometriosis
- chronic pelvic pain
- uterine prolapse
- cancers, such as uterine, ovarian, and cervical
What is a hysterectomy?
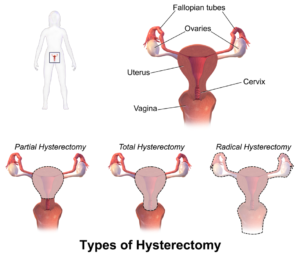
A hysterectomy is surgical procedure that removes the uterus (sometimes called the womb). There are 3 main types of hysterectomy.
- In a total hysterectomy, your doctor will take out the cervix and the body of the uterus together.
- If only the uterus is removed, but not the cervix, then it is called a partial or subtotal hysterectomy.
- In a radical hysterectomy, the uterus and neighboring tissues are removed, usually because there is a cancer present.
What other organs can be removed at time of hysterectomy?
Fallopian tubes and/or ovaries may be removed. If both fallopian tubes are removed, the procedure is called a bilateral salpingectomy. If both ovaries are removed, it is called a bilateral oophorectomy.
After a hysterectomy will I need to continue getting pap smears?
If the cervix is not removed, you will need to continue with cervical cancer screening. If the cervix is removed and you do not have a history of abnormal pap smears then you will not need to get pap smears. People with a history of abnormal pap smears who have had a total hysterectomy will need to discuss future pap testing with their doctor.
What are the different routes of hysterectomy?
The surgical route refers to how the surgeon performs the surgery. It is how the uterus is removed from the body.
- Vaginal hysterectomy – the uterus is operated on and removed through the vagina. The entire surgery is done through the vagina and there are no incisions on the abdomen.
- Abdominal hysterectomy – the uterus is accessed and removed through an incision on your abdomen.
- Laparoscopic hysterectomy – in this procedure, the surgeon operates with special instruments through 3-5 small incisions on your abdomen.
- Laparoscopic-assisted vaginal hysterectomy – this is a procedure that combines both laparoscopic and vaginal routes. This means that part of the surgery is done laparoscopically and the other part is done through the vagina.
- Robotic-assisted hysterectomy – The surgeon uses a special robot and works through multiple small incisions on your abdomen.
The laparoscopic and the robotic-assisted hysterectomies, and the vaginal hysterectomy are minimally invasive procedures.
What determines the route of hysterectomy?
This decision will be made by you and your doctor. Some of the factors that go into decision making include:
- the reason for the surgery
- whether other procedures need to be performed at the time of surgery
- history of previous surgeries
- other medical conditions like obesity
- availability of resources
- physician experience and skill
How long will I be in the hospital?
Your hospital stay depends on the route of hysterectomy, the extent of surgery and how you do after the surgery. With minimally invasive hysterectomies – laparoscopic, laparoscopic-assisted, robotic and vaginal hysterectomies—patients may be able to go home the same day or the day after surgery. Abdominal hysterectomies may require 1-3 nights in the hospital.
What should I expect?
You will not be allowed to eat food after midnight on the day of surgery. On the morning of surgery, you may have lab work performed if it wasn’t done before. If you are pre-menopausal, the nurse may do a pregnancy test to confirm that you are not pregnant. You will meet with your surgeon and the anesthesia team before being taken to the operating room.
After surgery you will likely be drowsy and feel tired. You may also feel some pain, nausea and vomiting. Your surgical team will work to ensure that you are comfortable and that your pain is well controlled. You may have a urinary catheter – a tube that drains your bladder. You may also have compression socks or devices on your legs that decrease your risk of blood clots. These will be removed once you are awake and able to walk around without help.
 At time of discharge from the hospital, your surgeon and nurses will discuss:
At time of discharge from the hospital, your surgeon and nurses will discuss:
- what activities you can do and what you should avoid
- what medications you can take for pain
- what signs or symptoms you need to watch for
- when to call the doctor when you are at home
You should not place anything in the vagina during your recovery period. Your doctor will tell you when you can resume sexual intercourse. You will also need to schedule a follow-up visit after surgery. Average recovery time from a hysterectomy is about 6-8 weeks. Your doctor will tell you when you can drive, return to work, exercise, have sexual intercourse, and when you can resume regular activity.
Lastly, your surgeon will advise you on any other additional issues specific to you.
What are the risks associated with hysterectomy?
Hysterectomy is generally a safe procedure. As with all surgeries there are risks such as:
- bleeding
- infection
- injury to neighboring organs
- inability to urinate
- blood clots
If your blood loss is large during the operation or if you develop symptoms from the blood loss, you may need a blood transfusion. There is a very small chance of getting an infection from the blood products. You may also need another surgery if there are complications after surgery.
There also some risks associated with receiving anesthesia. You will meet with your anesthesia team prior to surgery.
Take Home Points
- Hysterectomy – the surgical removal of the uterus – is one of the most common gynecologic surgeries performed today. It is done for reasons such as fibroids, heavy periods, prolapse, cancer, and many others. It is generally done when all other treatments no longer work.
- There are different types of hysterectomy. It may be done through the vagina, or through the abdomen using several small or one large incision. Sometimes only the uterus is removed, and sometimes the fallopian tubes and ovaries need to be removed as well.
- Hysterectomy is generally a safe procedure but does have some risks.
Author Information

Roseanne Gichuru, DO, MBA obtained her undergraduate degrees in Cellular Molecular Biology & Women’s Studies from West Chester University. She obtained her Medical Degree from Philadelphia College of Osteopathic Medicine and her MBA from St. Joseph University. She completed her OB/GYN residency at Crozer Chester Medical Center. She currently practices in PA. She has no disclosures to report.






